
Acceptance and Commitment Therapy for post-partum OCD: The transition to parenthood is difficult
When you have OCD, the transition to parenthood isn’t always easy. It can be particularly difficult when you suffer from post-partum OCD, which involves having obsessive fears about harming your baby because of an overwhelming sense of responsibility and duty toward your child.

Hit and Run OCD: Exposing Yourself to Your Fears
It’s Saturday morning and you’re sitting at home reading the paper. Suddenly your mind starts to play tricks on you, causing you to doubt your own experience. You start to doubt whether you did indeed turn the stove off before heading out the door, so you have no choice but to return home to check—even though logically you already know it should be fine…

The Importance of Seeing an OCD Specialist for False Memory OCD
If you suffer from what has been dubbed false memory OCD, it can be confusing to figure out if you actually have Obsessive Compulsive Disorder, or if what you are experiencing falls under an entirely different subtype.
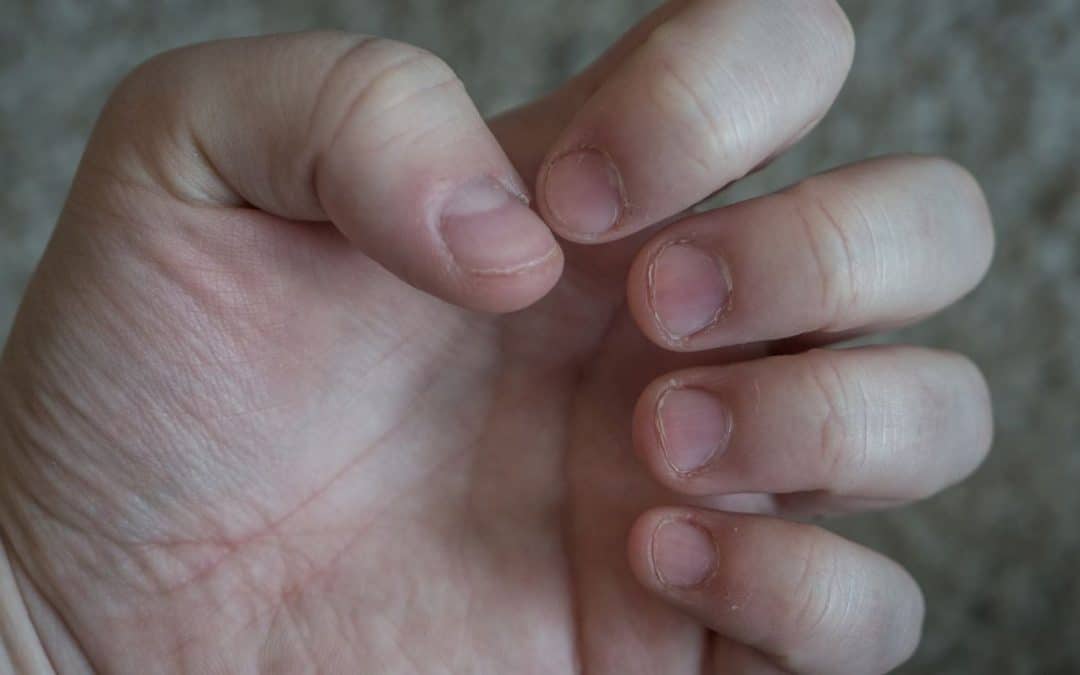
Can Habit Reversal Help Break the Cycle of Skin-Picking?
Skin-picking, also known as dermatillomania and excoriation, is a body-focused repetitive disorder (BFRD) in which the person has an irresistible urge to scratch, pick, or scrape their skin on a near-constant basis.

Depression: Effective Treatments including Acceptance and Commitment Therapy and Behavioral Activation
You know that you feel depression, and you may have even gotten treatment with pharmaceuticals or therapy. But what works to treat depression? We will look at the evidence behind Acceptance and Commitment Therapy (ACT) and Behavioral Activation (BA).
